|
It was 2015 and I was just getting started with my new practice. A breath of fresh air. After years of working inside the health system, I realized the focus is managing illness, not wellness. The focus was not on building relationships with your patients, getting to know them beyond the small talk, learning their story, meeting those who care for them, and definitely not on making health care delivery simple and efficient. I had no idea where this career move would go. I was nervous and scared of course, but happy.
I was rounding at the hospital as a hospitalist as I was still building my new practice when I met a wonderful young man. On my patient list it had said pneumonia as the reason for his hospital stay. I entered the room in my usual way, a knock, a wave, as I walked in with a big smile. “Hi there! I’m Dr Ahmed, just one of the hospital medicine doctors. How are you?” I said, not realizing my world was about to change. He managed to smile despite how ill he was from this long hospitalization. His family was at the bedside and greeted me upon entry. As this was my first time meeting him, I summarized his care so far to demonstrate to the family and him that I reviewed his chart in detail before coming so they can rest assured I will smoothly take over his care from my partner. He had an immune disease that made him susceptible to recurrent pneumonia. Each time he had pneumonia, the bacteria became more resistant to the antibiotics used to treat him that we literally came down to 1 antibiotic that would kill this bug. In addition, his lungs were getting scarred with each illness, leaving less viable lung tissue that could provide him oxygen. His family started to share his story. They shared with me how he has been battling not only his multiple pneumonias, but also his insurance company. They were taking him to multiple appointments between pulmonologists, infectious disease, immunologists, and multiple tests. The patient and his family could tell when a pneumonia was developing but by the time they would get a hold of the right doctor, he was already in trouble. He would be rushed to the ER. This routine was not only exhausting but kept putting him in the hospital. I listened to them carefully. By this time I had found a comfortable spot on the windowsill to sit. My brain was flooding with emotions. I was frustrated by the thought of this young man getting hospitalized multiple times and being away from family and friends. I was upset with the system that was not communicating properly and how difficult it was to get a hold of someone to get him the care he needed. If the family can tell when a pneumonia was starting, why was it so hard for them to get the treatment they needed to prevent a hospitalization? Then I was amazed. This young man still smiles and says “thank you” and “please” and “sorry to be a pest, but…” If I was in his shoes I probably would be upset and angry all the time! Not him. That was not in his DNA. He was different. He was unique. He was kind at heart. I slid off the windowsill as my mental clock screamed “Time is up! You need to see the rest of your patients! Hustle!” I fought this thought away and re-focused. You see, when you work in the system, we all have a mental clock that keeps us moving. Ten minutes here, five minutes there, this is how we get through rounds at a reasonable time with an average patient list of 15-18 patients all with multiple health issues happening at the same time. But, this time, I was different. I was not working for the system anymore so I was in charge of my time, not the system. I shared my practice with them and my frustration with the system. I told his family they are our teammates in caring for him. Therefore, all necessary resources must be readily available to them when they identify a health crisis is at hand. There should be no phone trees, voicemails, instead a human being there to help. That was my vision for health care. So I took him on as a patient in my private practice. I left the room with hope and determination to change the patient experience. In the following months and years, we battled his health insurance to cover an antibiotic that was the only one that would kill the bug causing his pneumonia. Several appeal letters were sent and we received denial after denial. His family, by the Grace of God, had a resource in the family who was able to get samples of this antibiotic. So, we hoarded this medication to treat him. It is absolutely amazing how the most powerful nation in the world allows its citizens to have to experience this much difficulty in seeking medical treatment. He went to Mayo in Minnesota and my team and I directly discussed his case with the team there. The Mayo team appreciated the communication and were able to treat him. He also was evaluated for a lung transplant. Initially he was denied and was high risk. We went to Texas for another opinion and they agreed to give him a chance with a lung transplant! I have to pause and share with readers how significant this is. I did a video call and he was in his apartment prior to transplant. He took multiple medications and nebulizer treatments just to keep breathing. His entire day was involved in helping his lungs oxygenate. Despite all of these challenges, he kept working at his job. He was determined not to miss work. Even when he was at the hospital, he would try to get work done. How incredible is that?? You have to understand, work gave him a purpose to fight and he deeply cared for his customers. He cared about his employer and his team. He embraced his responsibility. Throughout his illness, I was so amazed at how flexible his employer was with him. It seemed like the entire company were his cheerleaders and they were ready to help him along the way. It is a tremendous lesson for all employers. While I took care of his health issues, he was teaching me about resilience, kindness, the importance of having a positive mindset; and showing me how to treat my future employees and how important an organizational culture of compassion would be for my future team. It truly was a privilege and a blessing to have this incredible experience. After his lung transplant, he had about 2 years of incredible health. He was breathing better, having full conversations without coughing, walking without oxygen, and just doing great. My subsequent visit with him was incredible. Here is someone who would be constantly coughing throughout the conversation and now his voice was strong. Over the next few months, we started to develop a pneumonia here, a cough there, and he was treated accordingly. But, soon, on CT imaging, we started to see what we all feared. The scarring of his lungs started. It truly was a “oh shit” moment as I reviewed his images one day. Despite this, he battled with a smile and kindness. As a physician, there are times when you look at a radiographic image or set of lab results where you have a gut wrenching thought. While you wrestle this horrible thought, you become mindful of the surrounding glare from the patient and their family members. You have to quickly be mindful that although you have a bad feeling about something, you must reserve that thought until you complete the work up. Every physician has that feeling, that concern or belief, when they first see chaos on paper or radiographic image. At the same time, you must keep your composure and prepare the patient and their family members for what may lay ahead. After several more months, while I was rounding at the hospital, I received the dreaded phone call. As I was whooshing room to room like a downhill skier maneuvering the halls and going room to room, I stopped and stared at my phone. “LiveActive Member” it read. Before I answered the phone, I had a terrible feeling it was him. It was. He had called because he was having excruciating pleuritic chest pain. This was pain each time he took a breath. As his lungs expanded, the nerve fibers burned with pain signals bursting at the seams. He had this before and we were able to calm it down with medications, but this was different. He was screaming in pain and could not even complete his sentences. I calmed him down and knew this was a losing battle. We ultimately had to send him to the hospital. His oxygen needs increased while the team worked on his pain. He started to require very high concentration of oxygen. Even then, he was insistent on getting home so he can return to work. But his body would not comply. His lungs continued to fail and he agreed to hospice care while in the ICU. I finished up my last patient at the office and made the final click of my mouse to close all the windows on both computer monitors. I closed my eyes. It was an exhausting day. My wife, our Chief Operating Officer, came to my office. The two of us are the last to leave the office for many years. We both enjoy the quiet after hours that fill our office after our entire team heads home after a hard days work. "You should go visit him tonight," she said with a soft voice after she had settled quietly into one of the chairs across my desk. I was still staring at my black monitor screens, just exhausted from the day. My feet felt heavy. "I can drive and you just sit and relax. Or I can just go with you to keep you company!" She said in her usual upbeat excited voice. The two of us headed out, left her car in the parking lot, and got in my car to head to the hospital. Once we arrived to the ICU, I met his family and shared my condolences. I then walked over and held his hand. I was relieved. He was finally comfortable. He wasn't struggling to breath, he wasn't in pain. He was truly resting. He was on some sedative medications and on high flow oxygen. His family shared with me that they were trying to get him on lower oxygen to move him to the hospice floor and he was now full comfort care. While we visited, we shared stories, had some laughs as we reflected on some stories, and reflected on all the challenges we all went through while taking care of him. I turned towards him as I was saying goodbye to the family and noticed his chest rise was getting more spaced out. Something in my gut was telling me his time is very near. It was as if he was listening to our stories, our laughs, and when I stood up to leave, his soul was content and ready to move on. It was an incredible experience for me. As I said a final prayer for him, I left the room. My phone buzzed at 2 am. "LiveActive Member". It was his mother texting me that he had passed. You would think that I would burn out by allowing myself to be so close to my patients? It is actually the opposite. Prior to starting my private practice where I create real relationships with my patients, I was just working shifts. Getting through the day. When I did experience a patient death, it was usually anger. Why did the system not allow them to get their meds that may have caused this stroke or heart attack or preventing appropriate follow up, etc? Now, I have the privilege to battle with my patients. Fight for them, think with them, guide them as they navigate our health care maze. You feel you gave it your all and patients and their families take notice. You do it together. You battle together. What an honor and privilege to be part of such a significant aspect of human life. Why do physicians give up this incredible opportunity? How have we allowed the business of health care to become more like the manufacturing industry - volume over quality. And if quality is being incentivized, it is surrounded by heavy regulations where the cost of achieving quality service is greater than the reimbursement. So why do it? Our health care system is on the verge of massive change. Many physicians have already taken back control of their profession and career by going back to private practice. Ultimately, the support of our patients is what helps us achieve this goal. Your support, allows us physicians to think more clearly, give our patients a little more, strengthen our family bonds who support us and help us be most effective on a daily basis. As many thank you's I get from my patients family members, I tell them "No, thank you for supporting me to do this." - Dr Ahmed
0 Comments
February 1, 2015 was the day I broke free from the insurance run health care system. After several years of being a staff physician at a large health system, medical directorship, running research studies, writing articles, being a pharmaceutical consultant for 2 large companies, I realized I cannot change this system from within. Corporate greed was too great for a young physician to fight.
Each year I practiced medicine, I met another hard working American who waived his/her plastic insurance card, yet could not receive accessible or affordable primary care. I have met many other hard working Americans who couldn't get coverage regardless of the Affordable Care Act (ACA). The final story I could tolerate came when I met a 35 year old female who suffered a massive stroke and had to have her skull drilled to relieve the growing pressure from a massive brain hemorrhage. I took over her care after she had been moved from the ICU to the floor. My job was to figure out why she had the stroke, prevent the next stroke, and aggressively pursue rehab. I had triaged her as one of my last patients to see as she was reportedly stable. I knocked on the door and found a young brown haired caucasian female laying quietly in a dark room, alone. Her hair was disheveled as she had staples on one side of her scalp with part of her head shaved, allowing exposure to her staples. She looked exhausted. Unlike the other rooms, there were no flowers, no cards, no "Get Well" balloons. It was just her, a beeping IV pump, and a computer next to her bed. The guest couch and chairs sat empty in the corner of the room. The 42 inch TV was turned off. The large window provided some light as it penetrated the dark window and the window shade. Upon my entrance, she turned to look at me with sad eyes and managed to smile half way. I pulled up a chair next to her bed to listen to her story as I did with every patient. She readjusted herself, which was challenging as her entire right side was still weak. You see, she was a young 35 year old single mom who was working 3 part-time jobs, because her employers did not want to offer a full time job as that would require them to offer her health insurance under the current laws. So, she did not have insurance because of this. Her story began with a visit to an urgent care center where she was told she had high blood pressure and she was given a medication to help control her blood pressure. She didn't understand what high blood pressure would mean if it is not controlled. After taking the medication for a few days, she simply stopped taking it because to her it was all numbers and certainly didn't make her feel any "better." Besides, she was a young 35 year old and so how bad could it be? In reviewing her records, it seems she had presented to the ER with a blood pressure of 220/120. Likely, her blood pressure was the reason for her stroke and head bleed. The medication she was on for high blood pressure is $4. Needless to say, I can get this medication for my patients now for $0.87 for a month supply. As her story continued to unravel, I started to stoop lower and lower in my chair. My mind started to race with anger. How can she be so abandoned? Why did no one tell her about the importance of blood pressure? Where was the follow up visit? How is this fair? She is a contributing American citizen to our economy, yet we abandon her? To put all this in perspective, here she is as an uninsured patient with an ICU stay of 5 days, surgical drainage of blood, multiple imaging studies and labs, she couldn't move her entire right side and so will need 6-8 weeks of rehab. One of her jobs was being a waitress. There is no way she could return to this line of work. In essence, we have effectively bankrupted a young, sweet, innocent, 35 year old single mom. After she had completed her story, teary eyed, and by now I was almost laying in my chair, I straightened myself and leaned forward towards her. I said,"ma'am, I am so sorry for all this. We have failed you. I as a representative of the American health care system have failed you. For that, I am sorry." I went on to explain how important blood pressure is to control and how we can prevent another stroke. I left that room with only one thought in mind...NEVER AGAIN. Never again would I allow myself to be in that chair hearing a story like that from any of my patients. My mind was made up to offer the best primary care I can, regardless of insurance status. Many people do not hear the stories that we as physicians hear. Yes, you pay for insurance premiums, but for primary care, that insurance card likely is not getting you the best care. Think about it. Some pay $25 to over $100 in copay per visit for what? A 10-15 minute visit that feels rushed or is not comprehensive. Or be sent to a specialist, procedure, imaging study, or be prescribed pills when in reality you probably didn't need it. These decisions are made simply because there is no time to get to the root of the problem. The follow up is the most important component of primary care. Start a gameplan and then you need to follow up maybe in a week or 2 weeks. But eliminate the copays that people have to pay to make the follow up more feasible. This is where direct care makes sense and saves money. The young and healthy individuals also save money and gain value in a direct care model. Simply put, casting, medications, EKG, suturing is FREE or at a minimal cost in a direct care practice. Time and money is saved. But, think about the value. That young and healthy individual is probably going through some emotional roller coasters. What are their aspirations? How strong is their social network and who are they? Who do they spend time with and how are they dealing with any stressors they may have? Are they exercising and eating healthy? If they do exercise, then are they doing it safely? Do they practice safe sex? Where are they planning to travel? Are they overweight? Do they have family history of diabetes or heart disease that predisposes them to these conditions? These questions are so important that essentially a life can be saved by simply talking to them. These young adults are connected to their physician by a simple text or video chat under a direct care model. How neat is that? This is the value of direct care with or without health insurance. Take the time to understand what you are paying for when purchasing a health insurance plan. Our patients with Medicare and supplement insurance will say the value of access, coordination of care, and availability overwhelms the minimal monthly cost. Health insurance and direct care together make a phenomenal resource for all Americans to live well. Quality of life will be enhanced. Our health expenditures will go down. Taxes will be reduced and employers will be able to retain their talented workforce. Increase in direct care practices will solve the primary care shortage, lead to more young physicians embracing private practice to revive the practice of medicine, technology will be used to bring accessible health care into the home, and the American people will be empowered to navigate the health care system with more confidence. Together, we will achieve a healthier America. Give a direct primary care practice some consideration. Visit iwantdirectcare.com to learn where the nearest direct care practice is for you. Welcome to the new US Health Care System! Dr. Ahmed  The air was crisp this Sunday afternoon. The snow had already melted and the cold air brushed my face softly. My body was shaking from the cold, but my mind was too busy to really take notice. My shoes had managed to gather a layer of mud that was an inch thick. To my right and left, I was surrounded by sad faces. Many were people I have known from the community, my friends, and others I hope to know one day. As I looked around the muddy cemetery, I noticed the clean gray speckled tombstone blocks that were neatly organized in rows to identify where the deceased rested. However messy the grounds seemed, the tombstone blocks were clean as if it was a dry summer day. The trees were bare and the sun shined bright through a clear blue sky. At the distance I noticed the large fresh dirt mound that had been created to cover the deceased body whom we laid to rest this afternoon. All the sons surrounded the mound for their last prayers for their father. I could not help the tears that started to fill up. Why am I crying? I did not know the man. This was a very captivating moment for me. Here I am, extremely emotional for a man I never met, whom I never said a single word to, never shook his hand, never saw a picture of him till the announcement of his passing. What is the deal? Who I did know were his sons. You see, his children have impeccable personalities. When you meet them, your soul is fed with calmness, a certain ease, your heart slows a bit, and you can feel genuine compassion when they speak to you. I have watched, listened, and simply enjoyed being part of his son's community charity events. Their message is always simple and food for the soul: Live with compassion and use your talents to better your community. At least that is what they have taught me. You see, that is the mark of compassionate leaders - their actions touch us all in different ways. During the funeral, one of his sons educated us about his father. Most importantly, he said and I am paraphrasing "all the things we as sons do in the community and good deeds you see us doing, has been taught to us by our father." It was at that moment, I grasped what kind of man their father was. He was amazing. After listening to those words, I knew he was a great man. A humble man. A man who probably never made himself known in a room with a loud bolstering voice declaring all his accomplishments. Instead, I sensed he was a man who promoted a sense of community, provide a lending hand to those in need, emphasized the importance of charity - which comes in many forms, even a smile. It is these thoughts that came flooding in my mind with tremendous force. I could not handle the emotions that followed. It was a tsunami of thoughts and pictures of what I imagined him doing or saying to his adult children when they were young kids. I must say, I did well in fighting back the tears. But, as I lay down to sleep that Sunday night, the tears flooded my pillow. I could not fight it anymore. Silence of the night made the thoughts not only return, but were uninterrupted by any other concerns. The Abdullah brothers are an inspiration to me and to all of us. I am honored to know them and our Kansas City community is privileged to benefit from their extreme compassion. As a physician, they have taught me and motivated me to take my talents and skills to the next level to help those who are uninsured and insured to receive accessible and affordable primary care. I hope to be an asset to the community as the Abdullah brothers are to our community. When I pass, if my good deeds come even close to what their father has accomplished in raising his kids alone, then maybe, just maybe, I will get a chance to meet him...and thank him for his gift to my community. Dr. Ahmed  Many of you know I am very passionate about the practice of medicine and am quite vocal about how to improve our national health care system. There is one question that seems to be brought up consistently by my audience: How has the Affordable Care Act affected your practice? Furthermore, some people will ask, I have insurance so doesn't that mean I am covered? So, to clear the air on what is truly happening since the enactment of the ACA, I will attempt to explain it in simple terms in this blog post. Prior to the Affordable Care Act (ACA) being enacted on March 23rd 2010, physicians and economists have been yelling at closed ears about how expanding coverage is not the only solution to this mess. The 2 major problems in addition to coverage is ACCESS and COST of health care. Simply put, here is how the ACA impacted these key components of our health care crisis: COVERAGE: Although we have now insured an estimated 10 million of the 43 million who were uninsured, 18% of the US population uninsured down to 11%, we have accepted narrow provider networks, higher premiums, higher deductibles. The complexity of insurance products have increased, causing even more confusion as to what consumers are actually buying. In addition, there is confusion as to who is in your network and many consumers realized they have to travel significant distances to get care. The Commonwealth Fund found that the rise in premiums for employer-based plans had slowed in several states but they continue to rise faster than median income. Therefore, as wages stayed stagnant, premiums continued to rise. Finally, many providers do not participate in certain networks or insurance plans given their poor reimbursement. COST: Insurers can decrease or maintain a premium by shifting the out of pocket costs to the consumer, co-pays, and deductibles. Medications continue to rise in cost by double digits. Medicare premiums continue to rise and out of pocket expenses on average are $5,400 annually for the 65-70 year old, but increase substantially as we age given increased hospitalizations. The cost of medical devices and hospital stay continue to rise. Why do we have to negotiate these costs each time we review our hospital bills, which are full of vague charges? I have done outcomes research studies in a hospital setting where we try to show cost savings with a medical treatment. To estimate and create a line item cost of a single unit blood transfusion is impossible. ACCESS: Lack of understanding of networks, physicians not being part of poorly paying insurers, and the simple fact of increased demand with a decreasing supply of physicians has led to delayed diagnoses and even death. So, how has the ACA affected my direct primary care practice? Single answer: it has helped me from a business standpoint as our solution is even more significant and patients enjoy their freedom. The ACA has made it harder for those who are in the "donut hole" and their states have not expanded Medicaid to get any type of care other than our practice. In effect, our practice is saving the ER and the hospitals from ever increasing accounts receivables to writing off large amounts as charity care. From the PATIENTS PERSPECTIVE: Our practice provides accessible primary care services, urgent care visits, and affordable services whenever they need it. In addition, this relationship in the long term will prevent illnesses that cost Americans thousands of dollars. Finally, patients are empowered with resources to take care of themselves, they have transparent imaging, laboratory, and pathology pricing. They can CHOOSE to use their insurance for any ancillary service if they want and compare cash pricing to what the insurance companies will cover. From the PHYSICIAN PERSPECTIVE: The ACA has increased the red tape and regulations on medical practice. For example, on October 1, 2015 ICD-10 came into effect. The previous ICD-9 had 17,000 codes and this newer version has 141,000 codes! Think about the direct costs of software update, hiring more staff, and the indirect costs of training, lost revenue from inefficiency and slowed practice. Since we do not contract with insurance carriers, these nuances have no effect on us. The ACA has caused more physicians to leave the practice of medicine. There is an estimated deficit of 124,000 primary care physicians by 2025. Our practice has become more attractive where physicians can be sole owners of their practice and join Health Suite to share its resources and all of its community resources. Finally, the ACA motivated us to seek more partnerships to save our patients up to 95% on imaging, medications, and pathology for being our members. Bottom line: Practices like ours will soon be paired with high deductible plans, as they are in Washington state. This is low cost and high value for consumers. So, spend the time to look at our practice, talk with us, talk with our insurance brokers, save thousands of dollars for yourself or your company by pairing the right insurance product with our practice. Some good resources: NY Times article 2015 Milliman Medical Index Essay by Patrick Ishmael More employers shifting cost to employees So a couple of adventurous guys and myself thought we would head out to West Virginia to battle the infamous Gauley River. It is a 105 mile river that merges with the New River to form the Kanawha River, which is a tributary of the Ohio River. The Gauley River is the most popular advanced whitewater site in the country. It was a 2 day trip that involved piercing through challenging rapids that ranged from class 3-5. According to the American Whitewater Association, each rapid is ranked by the character of the rapid in terms of how violent and harsh it is, distance, technical difficulty to maneuver, and finally the difficulty of swimming in it. In other words, the higher the class of rapid, the higher the chance of something bad happening to you.
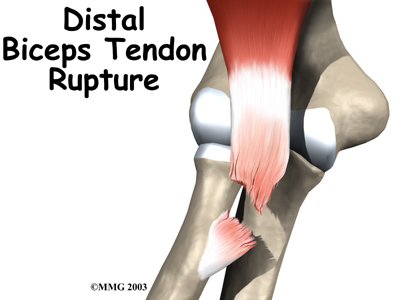
Check out the reviews: http://www.tripadvisor.com/Attraction_Review-g59234-d3330369-Reviews-New_Gauley_River_Adventures-Lansing_West_Virginia.html As you can see from the pictures, the river beat me up bad! I strongly recommend trying new sports and activities. Prior to this trip, my workouts were truly at its peak. Those of you who workout know what I am talking about. It is a point where lifts seem easier, body responds to the workouts, and each session is better than the previous. We all experience set backs and for me this really sucks! Quite honestly, my immediate thought was about how I cannot workout my upper body for several months. It really stinks. So you are probably wondering what happened? Well, it was the second day of the trip, the last class 5 rapid, and a huge rapid pushed me off the raft. This was the second time I was knocked off the raft and for some random reason, I thought I could grab a hold of the rope that was lining the outside of the raft to propel myself back onto the raft. The river, with all of its tremendous might kept pushing me away from the raft. The bicep muscle could not withstand the force and "pop" went the distal tendon. Ouch. Down I went with the river. If you have not gone rafting, this is the point of the story where all I remember is waves crashing on my face and seeing rocks zoom by as I continued to go down the river. This is where the only thoughts that go through your head is "I hope I don't hit a rock head first!" Luckily, I swam and navigated to the nearest raft and was lifted up onto safety by friendly strangers. I was surrounded by laughter and smiles as each patted me on the back. But, I could not smile. The pain was too intense. Life must go on. Today, at the clinic, I saw a few patients, ate lunch where I bumped into people I know who asked the obvious question after seeing my left arm in a sling "what happened?" It certainly makes for a good story. I must say though, my practice has spoiled me rotten. I cannot help but smirk when I have to fill out so many forms prior to seeing the doctor, go into the "second" waiting room only to get my vitals checked, then wait another 10 minutes before the doctor comes. The funny thing is, after all that, I was told I had to see another doctor since my muscle was so high up my arm after the tear. Ahh! Another visit, more forms, and more waiting! Will keep you posted on my progress. Please feel free to share your injuries with extreme sports or any sports injury. Injured, but always there for my patients, - Dr. Ahmed Recently, we had an urgent call where someone was in considerable amount of knee pain and requested our help in getting the right medical treatment for this knee pain.
LiveActive Primary Care jumped into action. Within an hour of taking the call, after evaluation of the knee, an MRI seemed necessary to further evaluate this knee. Their insurance carrier wanted prior authorization, which would delay the whole process, so we were asked to look for cash pricing. One institution quoted the MRI as a little over $3,000, whereas our imaging partner offered the same MRI, got him with a same day appointment and a same day read at a price of $400! That is a huge savings and considerably more efficient. The MRI was completed within an hour. A CD with uploaded MRI images was made and given to our client as they exited the imaging facility. In the meantime, we arranged an orthopedic consult within the next couple of hours. A report of the MRI was faxed to LiveActive Primary Care that same afternoon. Our client was seen by the orthopedist, the images were reviewed by the orthopedist, we had a copy of the MRI reports, and a complete evaluation with a treatment plan the same day! The total cost for the client was $400 out of pocket! Compare that to what would have happened in the traditional model: The client would most likely go the ER and have to fill out a bunch of paperwork. After an hour or 2, maybe more, they would then proceed to the exam room where they are asked several questions, intravenous fluids would be started, pain medications would be given - even tylenol in the ER is much more expensive than what you can buy at the store, a host of labs would be done. After answering the nurse's questions, they would answer the same questions AGAIN with an actual doctor. ER staff may proceed with an X-ray first and then later decide the client needs a follow up MRI as an outpatient since the MRI scanner is booked up with other patients. After another several hours, the client would leave with pain medications in hand, likely some combination of narcotics and tylenol to follow-up wth his primary care doctor. The total cost of this model, even suggesting that there was no MRI done in the ED would easily be thousands of dollars with insurance! More importantly, the case was simply evaluated on the surface only to delay the actual imaging that was needed with a high price tag; not to mention the amount of time that was wasted just waiting around for the evaluation to be done. Even if the ED cost is covered with Health Insurance, Medicare or cost is not an issue, the efficiency is incredible when we take away insurance and remove all the considerable barriers in our health system, which only impedes quality and efficient care delivery. That is the LiveActive experience! Our incentive is not to add services to make a profit; instead, our focus is on maximizing the patient experience with little to no cost for our members. Primary care should not be expensive and it most definitely should not be difficult to access. This is only one of many stories that we live everyday. Come join the movement in revolutionizing how primary care is done and experience the difference with LiveActive Primary Care! Did you know that the practice of internal medicine can be traced back to ancient India and China? In fact, the term Internal Medicine originates from the German term Innere Medizin. This term was popular in the 19th century and was brought to the United States from American physicians who trained in Germany in the early 20th century. The term Innere Medizin was used to describe physicians who combined the science of laboratory to patient care.
Internal Medicine physicians specialize in adult and geriatric medicine. So what defines "adult?" Well, nowadays that can be as young as 14 years old as kids are reaching adult weight of 50-70kg. In the past when I was in training we used to say anyone older than 16 or 18 years old. But, given the size of the average American, this definition has changed. I am comfortable seeing anyone who is "adult" weight. Therefore, I picked 14 years old as my starting age. You can twist my arm to see 13 year old folks... The American College of Physicians defines Internal Medicine as the following: "Internal medicine physicians are specialists who apply scientific knowledge and clinical expertise to the diagnosis, treatment, and compassionate care of adults across the spectrum from health to complex illness." So our favorite question is "why?" This used to drive my parents crazy when I was young. I was that annoying little one that always popped his head up and asked "why?" It is a lot of detective work and we love looking at data and forming hypotheses. We do not zone in on one diagnosis, but have a list of possibilities and eliminate each one as more clinical information becomes available. I feel like this is being lost in today's "hamster wheel" medicine where everyone is rushed and the average exam time is 7 minutes. We treat ear infections, eye infections, headaches, post stroke care, post heart attack, high cholesterol, diabetes, adrenal issues, thyroid issues, copd, asthma, pneumonia, skin infections, depression, anxiety, any mental disorder, arthritis, urinary tract infection, prostate issues, trouble urinating, impotence, diarrhea, constipation, any gasterointestinal diseases, arrythmia, heart failure....I think you get the idea. If the illness is beyond the scope of internal medicine or a special procedure is needed, a referral is made to a specialist. We are skilled in suturing, skin biopsy, skin tag removal, cautery, joint injections, some do botox injections and liposuction, and various other small office procedures. In addition, the major skill is prevention and early recognition of disease or pathology. So, coaching clients through current guidelines for screening for breast cancer, colon cancer, heart disease, high cholesterol, and much more is critical in the care of our community. This is what excites me about my new practice! As a hospital physician I treated post stroke care, acute heart attacks, head bleeds, severe infections with multi-organ failure and all that was gratifying. But, there were some cases where I would sit with my head in the palms of my hands thinking, "if only she had an internist or the internist had more time in taking care of her, or her medications would be affordable...if only..." I'll be honest, I did cry at times for my patients because many times it is not their fault. The system has failed them and they suffered such a catastrophic event that will only cost the system and more importantly the individual significant dollars. Thus, prevention, wellness, and being a coach is as, if not more important, than treating an acute illness. So when people ask, "why do I need an internist?" I usually tell them, "well you can get one when you get terribly sick in the hospital with a large bill or you can get one now and prevent a catastrophic event if possible." More importantly, life is about building relationships. The sooner you find an internist you like and can partner with, the better you will feel and likely live healthier. Statistics show that people do better with a good support system regardless of what the issues they are dealing with - medications are not always the answer. Sometimes people just need to talk. In my model, I will have time to listen. Maybe the anxiety or panic attacks you are experiencing is because of an acute issue you are dealing with. Does it make sense to prescribe an anti-anxiety medication in 7 minutes of hearing your story or does it make more sense to listen and see if we can work out a solution together and only prescribe if needed? I argue that these quick visits are leading to unnecessary prescribing, imaging, and laboratory - this all drives rising costs for everyone. I have passion for science and am amazed at our progress. But I also understand that there are things in this world that we still do not understand. Sure, not everything is in our control. But, I believe with the knowledge and technology that we have today, prevention of disease and the management of disease is not only our responsibility but it will allow us to take care of each other. As I tell all care-takers, you have to take care of yourself before you take care of others. We have to be there for each other and more importantly be healthy when we stand together; or else we both fall. Living healthy does not have to cost so much nor should it be a burden. So, join my practice and let's do this together! Let's live life to it's fullest and I will be honored if I can be your internist in this journey we like to call life! Your Internist, Dr. Ahmed |
Author"He who studies medicine without books sails an uncharted sea, but he who studies medicine without patients does not go to sea at all." Archives
March 2023
Categories
All
|
We are passionate about practicing medicine
|
|
CLINIC HOURS
MONDAY 9am-5pm TUESDAY 9am -5pm WEDNESDAY 9am-5pm THURSDAY 9am-5pm FRIDAY 9am-12pm Closed 12pm-1pm daily for lunch SAT&SUN CLOSED |
2024 Holidays - CLINIC CLOSED
New Year's - January 1st Memorial Day - May 27 Independence Day - July 4 & 5 Labor Day - September 2 Thanksgiving - Nov 27, 28 & 29 Christmas - December 24, 25 & 26 |
Contact Us
Tel: (913) 549-3884
Fax: (913) 273-3343
Email: [email protected]
6650 West 110th Street
Suite 220 A
Overland Park, KS 66211
Fax: (913) 273-3343
Email: [email protected]
6650 West 110th Street
Suite 220 A
Overland Park, KS 66211



 RSS Feed
RSS Feed