|
Have you ever wondered how this prescription drug abuse epidemic spiraled out of control? How did we let this happen? Who are the major stackholders? These powerful drugs were developed with a real noble purpose, but soon cycled out of control. Was it our own doing? Similar to cigarette companies, pharmaceutical executives have become significantly rich at the expense of bringing incredible harm to all of us. This is our terrible reality across all industries - greed always results in harming everyone involved. Physicians have been screaming about the dangers of these medications, but lawmakers continued to ignore them Why do we do this? Ignore the scientific community for the mighty dollar. Whether it be the approaching epidemic, rise of harmful medications or technologies, or gun control - the concern for financial profits always win. The commercial manufacturer of morphine started out in Germany in 1827. In fact, morphine was the painkiller of choice during the American Civil War. Interestingly, the doctor who invented Coca Cola formula had developed a morphine addiction during the Civil War and in their attempts to solve this issue, cocaine was sought. The new drink had cocaine mixed into it and sold to a pharmacy in Atlanta. During that time, this was perfectly legal. Heroin was created by Bayer Company in Germany in 1898. It's sole purpose was to be a remedy to the morphine addiction. Legislation, like The Pure Food and Drug Act of 1906 and Harrison Narcotic Tax Act in 1914, brought these addictive substances under the control of physicians; preventing casual distribution of these products. The current problem:
Factors that contributed to such growth:
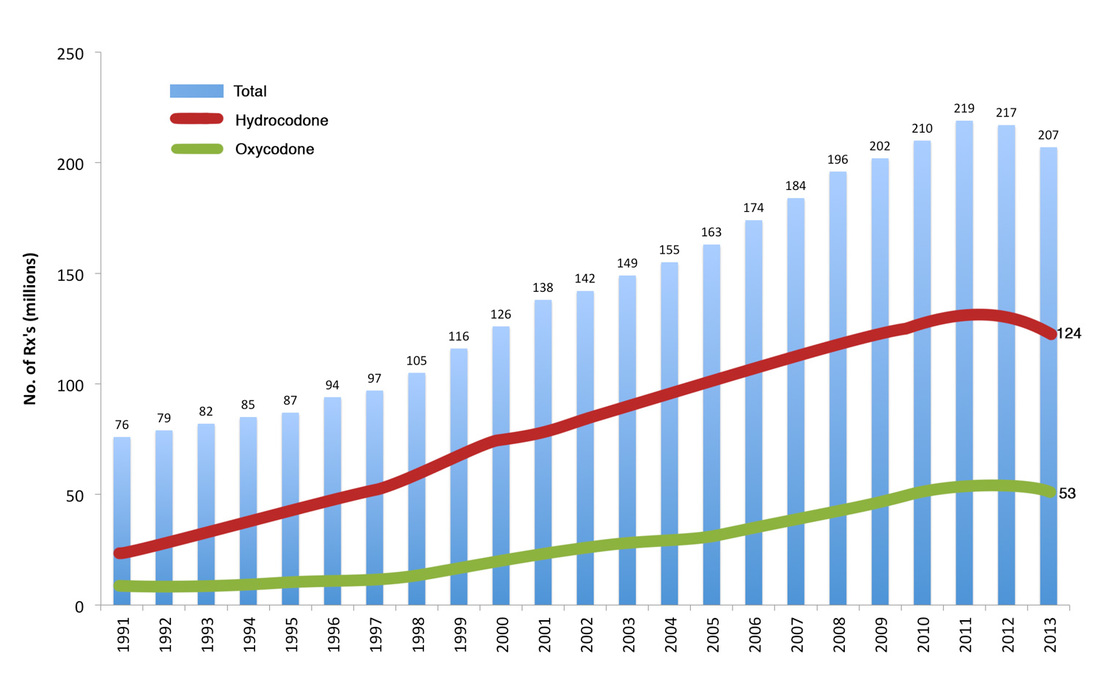
The number of prescriptions has increased from 76 million in 1991 to nearly 207 million in 2013. The United States is the biggest consumer globally. What does it mean for the pharmaceutical companies? It means more than $35 billion in sales since releasing medications like OxyContin. Annual revenues are about $3 billion for pharmaceutical companies selling prescription drugs. So, what does all this mean? Well, let's see... A medication or family of medications whose sole purpose was to help the soldiers during war starts to be sold unregulated to people around the world. Then as addiction starts to develop and people take notice, regulations are made to help control its spread, but either inadvertently or not, products like cocaine and heroin are used to "remedy" the situation. This leads to more addiction. Crap! Meanwhile, the US health system was undergoing major changes. In attempts to control costs in the 1960s-1990s major developments in public and private health plans were developed. Not too surprisingly, as the managed care organizations were attempting to control costs, US health expenditures started to rise, while reimbursement started to fall. Pharmaceutical companies started to market heavily and capitalized on a health care system that was reducing clinic visit times to an average 7-10 minutes, which led to more written prescriptions. Sound familiar? Our country has a HUGE antibiotic resistance problem where antibiotics are prescribed unnecessarily. The American public doesn't see the "super bugs" which claim many American lives where these bugs are resistant to ALL available antibiotics. Pharmaceutical companies do not invest in making more antibiotics as there is more money to be made in drugs that are taken for a long time, instead of the 5-7 days regimens that are usually prescribed for antibiotics. But, we digress. So what does the US government do to fight this epidemic? Spend more money where it doesn't matter! The President signed legislation that authorizes $181 million a year for new programs to train emergency personnel in administering drugs to reverse opiod overdoses and help communities purchase those drugs, as well as develop treatment and overdose programs. This means that pharmaceutical companies have more buyers for medications like Narcan and other products. Which leads to more profits! These treatment centers will be overwhelmed with the large demand as the public now has available "quick reversal" agents. This sends the wrong message and does NOT get to the root of the problem. Those of us who have taken care of overdose patients know that the problem does not cost so much money, development of more "reversal" agents, nor does it require capital investment to create "treatment facilities." The solution is simple: Establish a human connection involving time to talk, engage, motivate, build strong relationships, and bring people together. What does this solution look like more specifically? All physicians, including specialists, are demanding better primary care. Longer visits allow for conversation and developing a plan that may include various pain control options outside of prescription medications. The primary care setting is the place where opioid management should take place. Why not? The primary care physician is the leader of their care; the quarterback who is most likely or should be managing multiple health issues. They are the ones who spend time with the family, loved ones, might even have done a few house calls, knows what barriers exist to better health, and is the one making referrals or partnerships to bring more solutions to their delivery of care. This is what true primary care looks like. Not a place to get a referral to a pain specialist or some methadone clinic. Why do we accept such nonsense? Let the primary care doctor to what they are trained to do. The health system must support and allow this interaction to happen because this small investment will prevent huge costs in the future. Psychologists, counselors, psychiatrists, social work, and others might need to be involved. More importantly, there cannot be a delay in seeing each of these specialists and there needs to be total - 24/7 - contact between physician and patient to prevent "loss to follow up." This solution is cheaper, preserves human dignity, and most importantly it gets to the root of the issue - whether it be economic stress, poor family interactions or challenges, depression or other mental illness, or poor medical management of pain. I am optimistic that the American people will speak out and share their personal experiences with a direct primary care practice. Soon, the current momentum that is already motivating public and private insurance companies offering "total health " plans that has a direct care flavor or large health systems offering more ways for patients to connect with them, will lead to national support for direct care. The challenge will be for physicians to prevent corporate greed getting in the way of our patient care. To a healthier America, Dr. Ahmed
3 Comments
Memorial Day was originally established to celebrate Civil War heroes in a single unified day, instead of separate days celebrated by the Union and Confederate states. Around the 19th century, Memorial Day expanded to celebrate all veterans who fought as American forces. As physicians, we learn from one another and are united in our thirst for knowledge to better serve humanity . War, in all its ugliness and chaos, demands innovation in science and technology. Thus, it is not surprising that modern medicine seems to have strong roots during times of war. The ancient philosophers and scientists created a foundation for physicians during the Civil War to innovate to meet the demands of its wounded soldiers, but also to create standards of care that we practice even today. Here are 5 innovations that were developed during the Civil War: 1. LIFE SAVING AMPUTATION - The old practice of saving limbs with wound cleaning using rats and maggots was replaced with cutting off infected limbs to prevent the spread of infection. In fact, Union soldiers were known for amputations, had less mortality from their procedures, and took no more than 6 minutes to perform. The technique not to cut through joints and to cut far away from the heart as possible became the standard of care. 2. THE ANESTHESIA INHALER - Stonewall Jackson's surgeon recommended the removal of his left arm after it was injured during friendly fire. When a chloroform-soaked cloth was placed over his nose, General Jackson muttered, "What an infinite blessing," before going limp. The cloth was inefficient as the liquid evaporated quickly, so Dr. Julian John Chisolm invented a 2.5 inch inhaler. Chloroform was dripped through a perforated circle on the side onto a sponge in the interior - the patient inhaled through tubes and the vapors mixed with air. This new method required less liquid; thus, allowing the physicians to treat more soldiers and using less supplies. 3. CLOSING CHEST WOUNDS - Benjamin Howard, an assistant surgeon, was told to do busy work while his superiors performed the surgeries. He started to experiment and realized that if he closed the chest with staples and linen, the lungs did not collapse as they did when the chest cavity is opened from negative pressure; thus, there was no suffocation. Survival rates quadrupled with this new technique. This technique became the standard treatment. 4. FASCIAL RECONSTRUCTION Dr. Gurdon Buck, father of modern plastic surgery, looked onto a young 20 year old private named Carleton Burgan of Maryland. This private had battled pneumonia and now the mercury pills had led to gangrene that was moving from his mouth to his eyes. His right cheekbone had to be removed and the young man was willing to try anything to stop the infection. Dr. Buck was the first to photograph his progress of his repairs and use tiny sutures to minimize scarring.
5. THE AMBULANCE-TO-ER SYSTEM - The Union went into the First Battle of Bull Run on July 21, 1861 not expecting a true battle. As approximately 1,011 Union soldiers lay wounded, the ambulances remained empty, leading to high numbers of mortality. The civilian drivers at the time were, according to some, described as "cowards" or "drunkards." Jonathon Letterman, the medical director of the Army of the Potomac, created a model of triage that we all know today. He established caravans of 50 ambulances, each with a driver and 2 stretcher bearers. He hired private wagons to carry medical supplies. The ambulances had spring suspensions and a lock box to prevent soldiers from stealing protein, bedsacks, and morphine that was reserved for the injured. Every war brings innovation and the medical community must not forget the sacrifices made by soldiers, scientists, physicians, and several other professionals who made modern day medicine what it is today. In this reflection, we must ask the question, have we been effective in preserving that fundamental drive that our predecessors had to innovate to help a large number of people without regard to creating any complex systems that may interfere in allowing the injured to access the innovation? Memorial Day should make all of us pause and reflect on the many lessons learned across all professions during our times of war. What is even more fascinating is that those lessons continue to teach us today; regardless of how advanced we think we are as a society. In loving memory of all fallen soldiers, Dr. Ahmed |
Author"He who studies medicine without books sails an uncharted sea, but he who studies medicine without patients does not go to sea at all." Archives
March 2023
Categories
All
|
We are passionate about practicing medicine
|
|
CLINIC HOURS
MONDAY 9am-5pm TUESDAY 9am -5pm WEDNESDAY 9am-5pm THURSDAY 9am-5pm FRIDAY 9am-12pm Closed 12pm-1pm daily for lunch SAT&SUN CLOSED |
2024 Holidays - CLINIC CLOSED
New Year's - January 1st Memorial Day - May 27 Independence Day - July 4 & 5 Labor Day - September 2 Thanksgiving - Nov 27, 28 & 29 Christmas - December 24, 25 & 26 |
Contact Us
Tel: (913) 549-3884
Fax: (913) 273-3343
Email: [email protected]
6650 West 110th Street
Suite 220 A
Overland Park, KS 66211
Fax: (913) 273-3343
Email: [email protected]
6650 West 110th Street
Suite 220 A
Overland Park, KS 66211



 RSS Feed
RSS Feed